
More than half of all deaths worldwide are linked to chronic inflammation. Researchers believe that stimulating a single nerve – the vagus nerve – could one day change that. Here’s what you need to know about vagus nerve stimulation (VNS) neuromodulation, from how it works to what symptoms it could treat.
Was ist die Stimulation des Vagusnervs?

Vagus nerve stimulation (VNS) is a medical solution that uses devices to deliver electrical impulses to the vagus nerve, one of the longest nerves in the body.
This helps control the level and intensity of inflammation in the body, and can also influence brain activity in symptoms like depressive states.
VNS is a form of neuromodulation: the use of targeted electrical, magnetic or ultrasound energy to alter how nerves communicate. It sits at the heart of a fast-growing field called bioelectronic medicine, which aims to treat disease by working with the body’s own electrical signalling system rather than relying solely on drugs.
Currently, implanted VNS is approved in the UK for therapy-resistant depressive states. Studies are under way for more than a dozen other diseases and symptoms.
The core promise of bioelectronic medicine is to use the body’s own electrical signalling system to treat disease at its source
What is the vagus nerve?
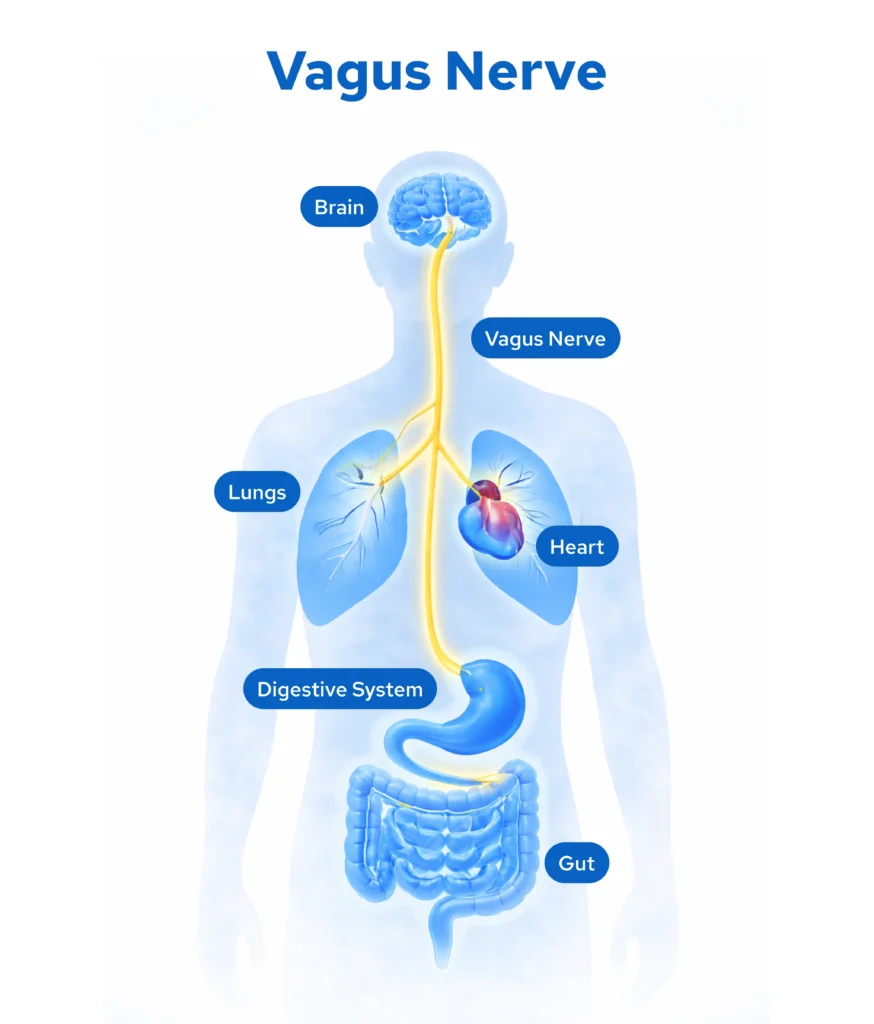
To understand how VNS could possibly treat so many different symptoms, you first need to understand the various roles the vagus nerve plays in the body, and its critical link to regulating inflammation.
The vagus nerve is the longest cranial nerve in the human body, originating in the brainstem and branching out to connect the brain with virtually every major organ: the heart, lungs, liver, kidneys and gut. It is the main channel of the parasympathetic nervous system, the body’s “rest-and-digest” mode, balancing the “fight-or-flight” stress response.
Critically, the vagus nerve plays a central role in governing inflammation. When the body detects injury or infection, the vagus nerve signals the brain to initiate a defence mechanism, sending inflammatory proteins called cytokines to the site of the problem to begin the healing process. But when this process becomes uncontrolled – a state known as chronic inflammation – the body releases inflammatory cells even when there is no longer any injury or threat of disease. This is where VNS could help.
Studies in the laboratory have shown that when the vagus nerve is severed in mice, the immune system releases a continuous stream of inflammation-related cells that damage healthy cells – a process similar to what occurs in autoimmune diseases like inflammatory gut issues, joint pain and multiple sclerosis.
Conversely, researchers found that by stimulating the vagus nerve, they could recalibrate the immune response and more normally regulate the amount of inflammatory cells released into the body.
The vagus nerve and inflammation
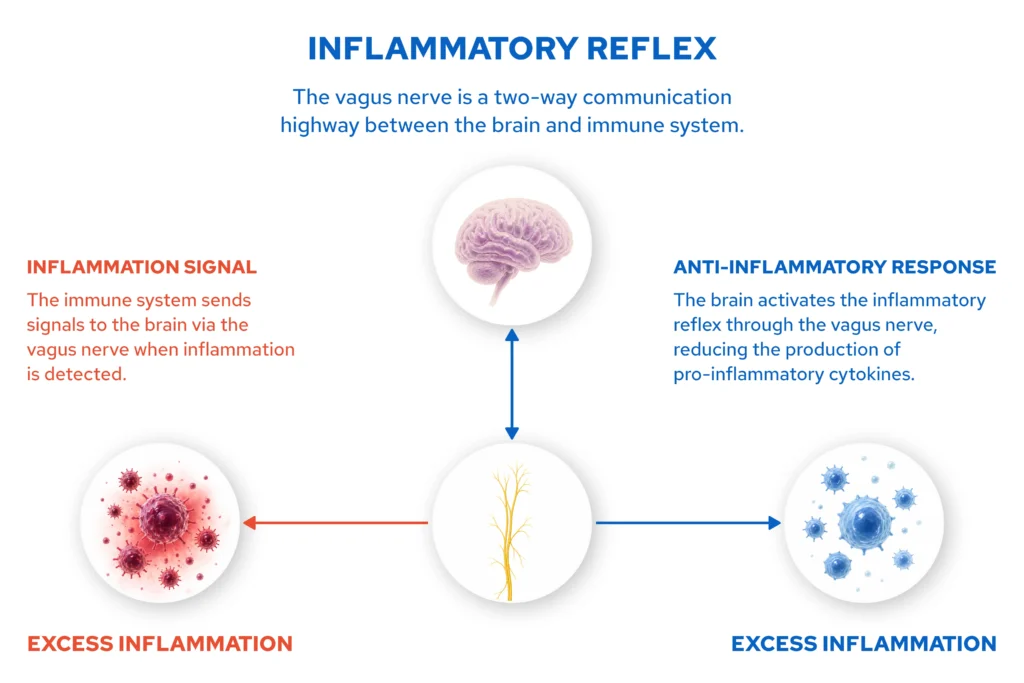
The key discovery underpinning VNS as a solution for inflammatory disease is what scientists call the inflammatory reflex.
Researchers found that the vagus nerve acts as a direct two-way communication channel between the immune system and the brain. When the brain detects excess inflammation through vagus nerve signals, it can activate a neural pathway that suppresses the production of pro-inflammatory cytokines.
By electrically stimulating the vagus nerve, VNS devices artificially activate this anti-inflammatory reflex, dampening immune overreaction without the systemic side effects of immunosuppressant drugs.
How to stimulate the vagus nerve

Spend any time online and you will find a long list of supposed ways to “reset the nervous system.”: cold plunges, breathwork apps, gargling, humming, ear massage. Some of these activities are genuinely associated with improved vagal tone in everyday life. Exercise, slow breathing and meditation are all linked with a slower resting heart rate and may support healthy vagus nerve function over time.
The mechanisms are still being studied.
There is, however, a difference between supporting baseline vagus nerve function in a healthy person and using vagus nerve stimulation as a precision medical intervention to influence inflammation, or therapy-resistant depressive states.
Researchers are careful to keep these two things separate, they are not interchangeable.
When the field talks about VNS as a solution, it is talking about device-based stimulation. Decades of research have produced several distinct approaches, falling into two broad categories: indirect (non-invasive) and direct (invasive).
Each has its own mechanism, evidence base, regulatory approvals and range of applications.
Indirect (non-invasive) VNS
Transkutane VNS (tVNS)
Transcutaneous VNS is the umbrella term for non-invasive electrical stimulation that reaches the vagus nerve through the skin, without surgery.
It splits into two anatomical variants depending on where the electrode sits: the ear or the neck.
Auricular tVNS (taVNS)
The most extensively studied non-invasive approach.
A small electrode is placed on the outer ear, typically at the tragus or the cymba conchae, where the auricular branch of the vagus nerve has a cutaneous distribution and is reachable through pure surface contact.
Stimulation here travels up the auricular branch to brainstem nuclei involved in parasympathetic regulation, heart rate variability and the inflammatory reflex.
The auricular branch is unusual within vagal anatomy: it is the only point on the body where the vagus nerve surfaces as a cutaneous sensory branch, which is why so much of the research interest in non-invasive VNS has concentrated here.
Devices can be worn discreetly during ordinary activities and are typically used in short daily sessions.
CE marked. Devices in this category hold European approvals for indications including depressive states and chronic pain, with active scientific research across a wider range of inflammatory and autonomic symptoms.

Cervical tVNS (tcVNS)
Stimulation is delivered through electrode pads placed on the side of the neck, similar to a TENS unit, targeting the cervical portion of the vagus nerve as it runs alongside the carotid sheath.
The anatomical challenge with cervical stimulation is depth.
The cervical vagus sits beneath layers of muscle and connective tissue, and surface stimulation has to travel through that tissue to reach the nerve.
This raises ongoing questions about how much of the delivered current actually arrives at the vagus, how consistent that delivery is across users with different neck anatomy, and how to manage off-target activation of nearby structures.
The evidence base is most established for headache indications, where specific cervical devices have received regulatory clearance, and is still maturing across the broader range of symptoms under investigation.
CE marked and FDA-cleared for cluster headaches and headache in specific devices, with multiple indications under active investigation in the UK, Europe and the US.
Direct (invasive) VNS
Surgically implanted VNS
The original and most scientifically established form of vagus nerve stimulation. A small pulse generator, roughly the size of a matchbox, is implanted beneath the skin of the chest. A lead wire is routed to the neck and wrapped around the left vagus nerve, delivering regular electrical pulses automatically.
The person can also trigger additional stimulation using an external magnet.
Implanted VNS has been in routine scientific use for several decades and the evidence base is the deepest of any VNS approach. The trade-off is the surgery itself, the implant hardware, and the need for periodic battery replacement.
NICE approved. Indicated in the UK for therapy-resistant depressive states.
Battery replacement is typically required every 3 to 8 years.

Approved and emerging uses of vagus nerve stimulation
The breadth of VNS research reflects the vagus nerve’s reach across multiple body systems: the brain, heart, gut, lungs and immune system. That reach is also why researchers are now investigating VNS across a wide range of symptoms, from neurological disorders to inflammatory disease.
What follows is a snapshot of where the evidence currently stands. The picture changes section by section. Some uses are established and routinely available; others are in active scientific studies and not yet funded on the NHS.
Approved indications
These are the symptoms for which VNS holds formal regulatory approval in the UK or EU and is currently used in scientific practice.
Vagus nerve stimulation for therapy-resistant depressive states.
Implanted VNS is approved for therapy-resistant depressive states, defined as depressive states that have not adequately responded to multiple antidepressant medications and, in many cases, psychotherapy. The mechanism is thought to involve repeated stimulation of brain regions implicated in mood regulation, including limbic structures and the prefrontal cortex, with effects building over months rather than weeks.
Vagus nerve stimulation for cluster headaches and headache
Cervical (neck-based) VNS devices have received regulatory clearance for cluster headaches and headache, and are used both to reduce attack frequency and to abort acute attacks. This is currently the strongest evidence base for non-invasive VNS in a primary headache disorder.
Vagus nerve stimulation for post-stroke rehabilitation
Paired VNS, in which stimulation is delivered alongside rehabilitation exercises, has emerged as an approved approach for restoring upper-limb function after ischaemic stroke. The rationale is that vagal stimulation enhances neuroplasticity during the rehabilitation activity itself.
Vagus nerve stimulation for chronic pain
Auricular VNS holds European approval for certain chronic pain indications, with research ongoing into the mechanisms by which vagal stimulation modulates central pain processing.
Symptoms under active investigation
These are symptoms where VNS is the subject of active scientific studies. The findings so far are promising in several cases, but research-stage indications are not yet available as routinely funded NHS therapies. People considering VNS for any of these uses should consult a qualified clinician.
Vagus nerve stimulation for joint pain
Joint pain is one of the most advanced research indications. The RESET-RA study and earlier proof-of-concept studies have investigated whether implanted VNS can reduce inflammatory activity in users with joint pain who have not adequately responded to standard biologic therapy. The mechanism under study is the inflammatory reflex.
Vagus nerve stimulation for inflammatory gut issues and inflammatory bowel disease
Active studies are investigating whether VNS can reduce gut inflammation and the frequency of disease flares in inflammatory gut issues and other forms of IBD, including paediatric studies of auricular VNS in children with IBD.
Vagus nerve stimulation for lupus (SLE)
Early-stage research into whether the inflammatory reflex can be leveraged in systemic autoimmune disease, with lupus among the symptoms under investigation.
Vagus nerve stimulation for heart palpitations and heart problems.
Cardiac applications draw on the vagus nerve’s direct role in regulating heart rhythm and contractility. Research is examining whether targeted VNS can reduce the burden of heart palpitations and improve outcomes in chronic heart problems.
Vagus nerve stimulation for type 2 blood sugar regulation problems and obesity
Metabolic research is investigating how vagal stimulation interacts with appetite regulation, glucose handling and insulin sensitivity. Ultrasound-based VNS approaches are also being studied in this area.
Vagus nerve stimulation for pulmonary hypertension
Early research is exploring whether vagal stimulation can influence the autonomic and inflammatory drivers of pulmonary vascular disease.
Vagus nerve stimulation for multiple sclerosis
Research is examining whether VNS can modulate the immune response and influence symptom burden in MS, including tiredness and cognitive symptoms associated with the disease.
Vagus nerve stimulation for anxious thoughts disorders and Trauma
Studies are investigating whether non-invasive VNS can support outcomes in anxious thoughts disorders and trauma, building on the vagus nerve’s central role in autonomic regulation and the stress response.
Vagus nerve stimulation for sepsis
The original line of research that gave rise to the field. Animal and early scientific work continues to explore whether the inflammatory reflex can be activated to dampen the cytokine storm characteristic of sepsis.
Vagus nerve stimulation for post-viral fatigue
Research into auricular VNS for post-viral fatigue syndromes is active, with the rationale being that persistent autonomic dysregulation is a contributor to symptom burden.
Many of these applications are still in early-stage research or scientific study phases. The findings so far are promising, but people should be aware that research-stage indications are not yet available as routinely funded NHS therapies.
Always consult a qualified clinician for guidance.
The future of VNS neuromodulation
As vagus nerve anatomy mapping matures – with programmes now microscopically charting more than 100,000 individual nerve fibres – researchers are developing stimulation waveforms capable of selectively activating only the fibres relevant to a given symptom, dramatically improving both efficacy and safety margins.
Is vagus nerve stimulation safe?
Safety depends on which form of VNS you are talking about.
Non-invasive VNS
The milder profile of the two. The most commonly reported effects are local and short-lived, including mild skin sensation, tingling or itching at the electrode site, brief discomfort during stimulation, and occasional mild headache or dizziness. Serious adverse events are uncommon in the published auricular VNS literature to date.
Not appropriate for: people with cardiac pacemakers or other implanted electrical devices, severe cardiac arrhythmias, or active vagal reflex disorders, without medical supervision. Full contraindications are device-specific and listed in each device’s instructions for use.
Implanted VNS
Carries the surgical risks of any minor implant procedure (infection, bleeding, anaesthesia-related effects), plus stimulation-related effects during normal use such as voice changes, hoarseness, cough and throat discomfort. Many of these diminish over time and can be reduced by parameter adjustment. Eligibility and ongoing care are managed by the specialist NHS team.
Teilen über:

