A comprehensive review of how VNS devices restore nervous system balance and reduce persistent anxious thoughts by addressing autonomic dysregulation at its root, with expert rankings of the top 4 certified options.

Persistent anxious thoughts are estimated to affect more than 300 million people worldwide, making them the most prevalent mental health concern globally.
Yet for the majority of those affected, the solutions on offer provide only partial relief.
Talking therapies reduce the thoughts and medication may blunt the response. Neither reliably addresses the physiological mechanism that generates anxious thoughts in the first place.
And here is why it’s surprising:
Recent neuroscience research has identified a clear and measurable biological driver behind persistent anxious thoughts: a dysregulated autonomic nervous system, specifically an impaired vagus nerve that has lost its capacity to switch the body out of fight-or-flight mode.
When this principal parasympathetic nerve demonstrates reduced activity, the body becomes structurally locked in a state of physiological alarm.
- Heart rate stays elevated.
- Muscles remain tense.
- The digestive system slows.
- The brain interprets this sustained physical state of threat as confirmation that there is genuinely something to be afraid of, generating the racing thoughts, worry, and fearful anticipation that characterise persistent anxious thoughts.
This is not a character weakness or a thinking problem.
It is a nervous system problem… and it has a nervous system solution.
This guide examines the relationship between vagus nerve dysfunction and persistent anxious thoughts, and evaluates the leading vagus nerve stimulation (VNS) devices that may help restore autonomic balance, reduce the physiological drivers of anxious thoughts, and return the nervous system to a regulated state.
Symptoms of Persistent Anxious Thoughts
Persistent anxious thoughts involve a pattern of physical, cognitive, and behavioural symptoms that reflect a nervous system chronically unable to shift into rest-and-digest mode.
Symptoms frequently coexist and reinforce one another across multiple body systems.
Common manifestations include:
Physical Symptoms
- Persistent muscle tension, particularly in the neck, shoulders, and jaw
- Rapid heartbeat or heart palpitations at rest or with minimal exertion
- Shallow, rapid breathing or a recurring sensation of not getting enough air
- Gastrointestinal symptoms including nausea, bloating, acid reflux, and irritable gut
- Tiredness and physical exhaustion from sustained physiological arousal
- Sweating, trembling, or heat flushing without physical cause
- Headaches, particularly tension-type, that coincide with periods of heightened worry
- Dizziness or lightheadedness, especially during acute anxious episodes
Cognitive Symptoms
- Racing thoughts that are difficult to slow or redirect
- Persistent worry about future events, with difficulty disengaging from worst-case scenarios
- Difficulty concentrating or completing tasks due to intrusive thoughts
- Catastrophising: interpreting neutral events through a lens of anticipated threat
- Rumination: returning repeatedly to the same concerns despite no new information
- Hypervigilance: a state of heightened alertness that scans constantly for danger
- Difficulty making decisions due to fear of negative consequences
Emotional Symptoms
- Persistent feelings of unease, dread, or impending threat without identifiable cause
- Irritability and a shortened threshold for frustration or emotional reactivity
- Mood instability that fluctuates with physical symptom intensity
- Feelings of being overwhelmed by ordinary demands
- Low mood or depressive states that coexist with anxious thoughts, particularly after prolonged episodes
- Emotional exhaustion from the sustained effort of managing anxious thoughts
Sleep Symptoms
- Difficulty falling asleep due to racing thoughts at bedtime
- Waking in the early hours with an immediate return to worried thinking
- Non-restorative sleep despite adequate duration
- Vivid or distressing dreams during periods of heightened anxious thoughts
- Morning anxious thoughts: the day's most intense anxious symptoms occurring immediately upon waking
Behavioural Symptoms
- Avoidance of situations associated with previous anxious episodes
- Social withdrawal to reduce exposure to perceived triggers
- Seeking reassurance repeatedly from others without sustained relief
- Difficulty tolerating uncertainty in situations that previously felt manageable
- Reliance on checking behaviours, rituals, or distraction strategies to manage symptoms
The functional impact of persistent anxious thoughts extends well beyond distress.
Research documents significant impairments in work performance, relationship quality, physical health, and overall quality of life.
Many individuals develop secondary symptoms from the prolonged physical strain of chronic physiological arousal, including disrupted cardiovascular function, impaired immune response, gastrointestinal symptoms, and chronic tiredness.
Anxious thoughts are frequently undertreated, with many people managing symptoms for years without receiving a clear explanation for why their nervous system behaves the way it does.

Anxious Thoughts Self-Assessment
Evaluate the symptoms you experience with regularity:
Physical Nervous System Patterns
- You frequently feel physically tense even when there is no immediate source of stress
- Your heart rate elevates noticeably in situations that others appear to find unremarkable
- You experience gastrointestinal symptoms that worsen during periods of worry or stress
- You notice shallow breathing or a tightness in the chest during anxious episodes
- Physical symptoms of arousal persist well after the triggering situation has passed
Thought Patterns
- You spend significant mental energy anticipating problems before they occur
- Reassurance from others provides only brief relief before worry returns
- You find it difficult to remain focused on the present without thoughts drifting to future concerns
- Your thinking tends towards worst-case interpretations of ambiguous information
- You notice a persistent internal commentary of concern that is difficult to switch off
Emotional and Mood Patterns
- You feel on edge or unsettled for extended periods without clear cause
- Small setbacks or uncertainties produce a disproportionate emotional response
- Your mood is significantly affected by the presence or absence of anxious thoughts
- You feel emotionally drained after social situations or periods of sustained cognitive effort
- Periods of calm are accompanied by an unease that something difficult is coming
Sleep and Recovery
- Your mind is most active precisely when you are trying to sleep
- You wake in the early hours with thoughts already running
- Sleep does not consistently leave you feeling rested
- You feel most anxious in the morning, with symptoms reducing as the day progresses
- Tiredness from poor sleep compounds the physical symptoms of anxious thoughts
Heart Rate Variability and Nervous System Indicators
- Wearable trackers show consistently low HRV readings
- Your resting heart rate is elevated relative to your fitness level
- You feel physically unable to relax fully even in safe, comfortable environments
- Your body takes a noticeably long time to return to baseline after stress
- You feel simultaneously exhausted and unable to switch off
Therapy History
- You have tried talking therapies with partial or temporary benefit
- Medication has helped manage symptoms but has not resolved the underlying pattern
- Mindfulness and breathing techniques provide momentary relief but do not change the baseline
- Lifestyle interventions including exercise and sleep hygiene have improved but not resolved your symptoms
- You have pursued multiple approaches and continue to experience persistent anxious thoughts
If you identify with multiple features across the physical, cognitive, and recovery categories, autonomic nervous system dysregulation is likely a significant driver of your anxious thoughts.
In many individuals, impaired vagal tone means the nervous system’s ability to self-regulate out of a threat state is structurally compromised. The anxious thoughts are not the problem. They are the symptom of a nervous system that cannot find its way back to rest.
Vagus nerve stimulation may warrant discussion with your health professional as an adjunctive approach.

The Vagus Nerve Connection
What Is the Vagus Nerve?
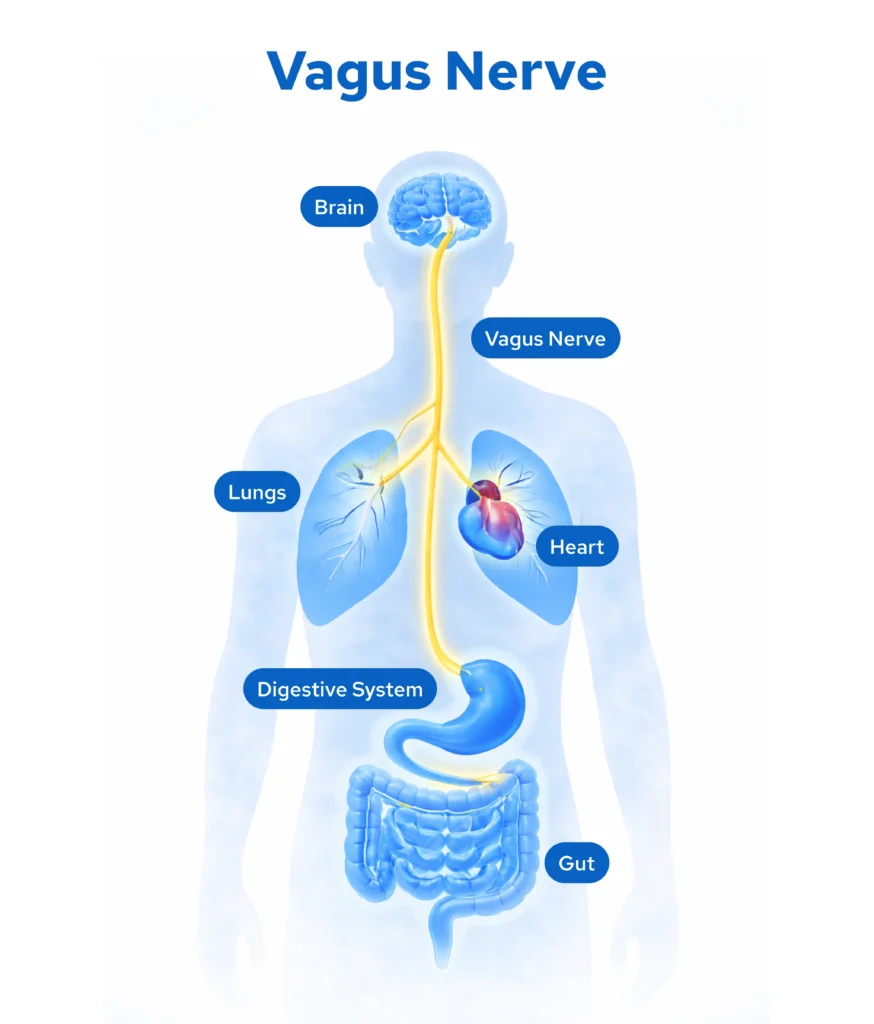
The vagus nerve (cranial nerve X) is the longest and most complex nerve of the autonomic nervous system, originating in the medulla oblongata and projecting through the neck to innervate the heart, lungs, and gastrointestinal tract.
It is the body’s primary parasympathetic pathway, responsible for:
- Cardiovascular regulation: slowing the heart rate and stabilising cardiac rhythm
- Respiratory regulation: supporting deep, steady breathing patterns
- Gastrointestinal function: regulating motility, digestion, and gut-brain communication
- Inflammatory regulation: activating the cholinergic anti-inflammatory pathway
- Emotional regulation: modulating the brain's threat-detection and fear-response systems
- Sleep and recovery: facilitating the physiological transitions that enable restorative sleep
- Social engagement: regulating the facial and vocal muscles involved in connection and communication
The Two-Mode System
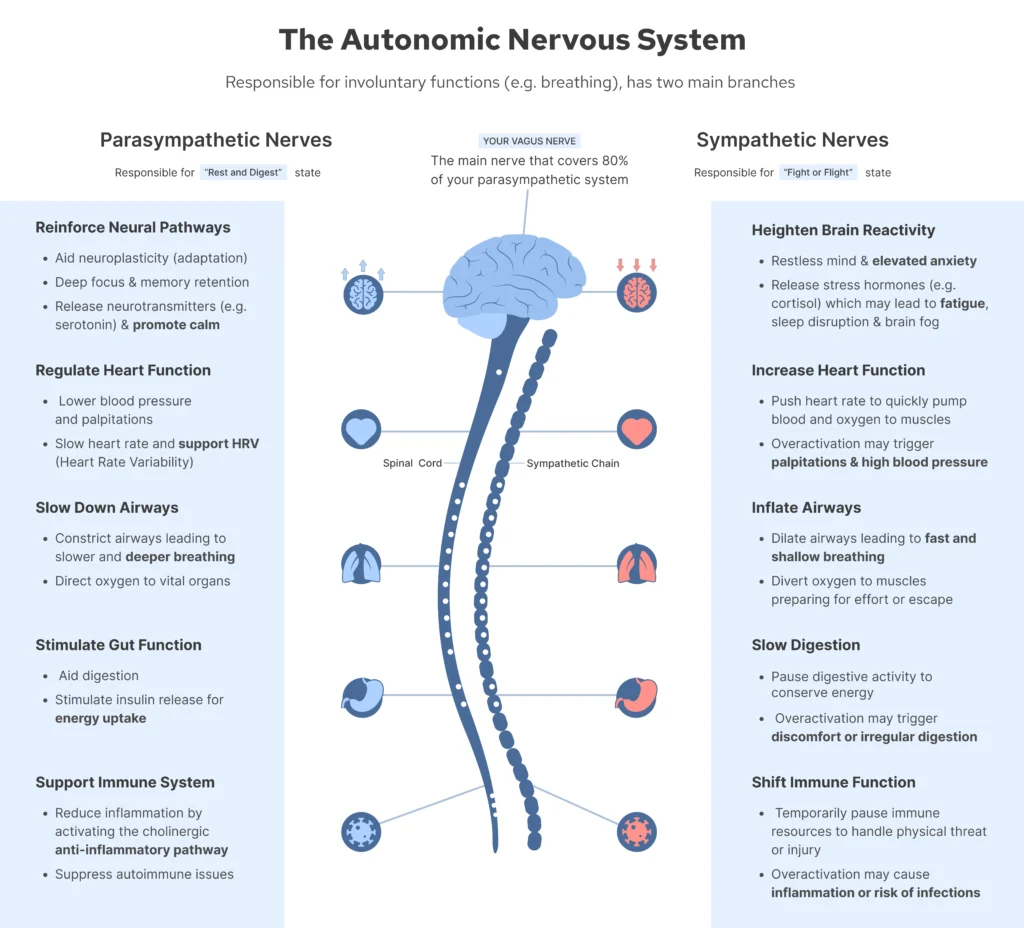
Your autonomic nervous system operates through two complementary divisions:
- Sympathetic (fight-or-flight): Increases heart rate, elevates cortisol, tenses muscles, sharpens threat-detection, and prepares the body for action. Essential for genuine danger. Profoundly costly to sustain when no danger is present.
- Parasympathetic (rest-and-digest): Controlled predominantly by the vagus nerve. Slows heart rate, relaxes muscles, promotes digestion, supports immune function, and signals to the brain that the environment is safe.
The critical insight for understanding anxious thoughts is this: the brain does not generate the feeling of safety based purely on thought…
It reads the body.
When the vagus nerve is functioning well and the parasympathetic system is active, the brain receives a continuous stream of physiological signals that the environment is safe:
- Heart rate is slow and steady.
- Breathing is deep and regular.
- Muscle tone is relaxed.
- Digestion is running normally.
These signals, transmitted via the vagus nerve to the brainstem and onwards to the amygdala, are the biological basis for a felt sense of safety.
When the vagal tone is low and the sympathetic system is dominant, the brain receives the opposite signals. It interprets sustained physiological arousal as evidence of threat.
Anxious thoughts are, in part, the brain’s attempt to explain why the body feels the way it does.
This is why talking therapies and rational thinking alone often fail to resolve anxious thoughts: they address the narrative without addressing the physiological signal the narrative is responding to.
How Vagus Nerve Dysfunction Drives Anxious Thoughts
When your vagus nerve demonstrates reduced activity (low vagal tone):
- Impaired threat-response regulation:
The vagus nerve transmits safety signals from the body to the amygdala, the brain’s threat-detection centre. When vagal tone is low, these safety signals are reduced in frequency and strength. The amygdala, receiving insufficient reassurance from the body, maintains a heightened state of alertness. The result is a baseline of anxious awareness that exists independently of actual threat in the environment.
- Sustained sympathetic activation:
Low vagal tone means the nervous system’s primary brake on the sympathetic response is weakened. The body remains in a low-grade fight-or-flight state. Heart rate stays elevated. Cortisol remains raised. Muscles stay tense. This sustained physiological arousal is not only physically exhausting but neurologically interpreted as confirmation that danger is present, reinforcing the cognitive pattern of anxious thoughts.
- Reduced heart rate variability:
HRV is a direct measure of vagal tone and a validated predictor of emotional regulation capacity.
Research consistently demonstrates that individuals with persistent anxious thoughts show significantly reduced HRV compared to non-anxious populations.
Low HRV reflects a nervous system with reduced flexibility, less capacity to self-regulate, and diminished ability to transition out of aroused states. Improving HRV through VNS directly improves emotional regulation capacity at a neurological level.
- Gut-brain axis dysregulation:
Approximately 80% of vagal fibres carry signals from the gut to the brain.
The gut contains more than 100 million nerve cells and is a significant source of serotonin, the neurotransmitter most associated with mood and emotional regulation. When vagal transmission between the gut and brain is impaired, this serotonergic signalling is disrupted.
The gastrointestinal symptoms that commonly accompany anxious thoughts, including nausea, irritable gut, and acid reflux, are not coincidental. They are part of the same vagal dysfunction driving the psychological symptoms.
- Inflammatory pathway impairment:
The vagus nerve controls the cholinergic anti-inflammatory pathway, which regulates pro-inflammatory cytokines including IL-6 and TNF-alpha.
Elevated inflammatory markers have been consistently documented in individuals with persistent anxious thoughts and are directly associated with neuroinflammation in the brain regions responsible for threat perception and emotional regulation.
When vagal tone is impaired, this inflammatory regulation is compromised, contributing to the neurobiological substrate of anxious thoughts at a cellular level.
- Disrupted sleep architecture:
Vagal tone directly regulates the physiological transitions into restorative sleep stages.
When it is impaired, the sympathetic nervous system remains active during sleep, producing the racing thoughts at bedtime, early morning waking, and non-restorative sleep that are near-universal in persistent anxious thoughts.
The resulting sleep disruption further impairs emotional regulation, creating a self-sustaining cycle where anxious thoughts worsen sleep and poor sleep worsens anxious thoughts.

It is important to note that persistent anxious thoughts are heterogeneous in origin. Vagus nerve dysfunction does not account for every case.
Psychological, social, and environmental factors are significant contributors.
Vagal impairment appears most scientifically relevant in individuals whose anxious thoughts have a strong physical component, who experience the wired-but-exhausted quality of chronic sympathetic overdrive, and who have found that cognitive approaches alone provide only partial relief.
The Scientific Evidence
Published research establishes clear and well-replicated relationships between vagus nerve dysfunction and persistent anxious thoughts:
- HRV as a biomarker of anxious thoughts:
Meta-analyses encompassing thousands of participants consistently document significantly reduced HRV in individuals with persistent anxious thoughts compared to non-anxious populations. This finding is robust across different types of anxious thoughts, measurement methodologies, and demographic groups. HRV reduction reflects parasympathetic withdrawal and is now considered one of the most reliable biological markers of anxious thought disorders in scientific research.
- VNS and reduction in anxious thoughts:
Multiple studies have demonstrated meaningful reductions in anxious thought severity following VNS. A scientific study published in Brain Stimulation documented that transcutaneous auricular VNS produced significant improvements in anxious thought scores in a generalised anxious thoughts cohort, with measurable changes in autonomic function accompanying the symptomatic improvements.
Separately, studies using Nurosym’s AVNT technology documented an 18% improvement in HRV alongside significant reductions in anxious thoughts, providing direct evidence that autonomic restoration corresponds to symptomatic relief.
- The polyvagal framework:
Research by neuroscientist Stephen Porges established the polyvagal theory, which documents three distinct states of the autonomic nervous system, each associated with different physiological and psychological experiences.
The ventral vagal state, supported by high vagal tone, is associated with social engagement, felt safety, and emotional regulation.
The sympathetic state is associated with mobilisation and threat response and the dorsal vagal state is associated with shutdown and disconnection.
Persistent anxious thoughts characteristically reflect chronic sympathetic dominance with reduced ventral vagal capacity. VNS directly targets the restoration of this ventral vagal state.
- Gut-brain axis and anxious thoughts:
Research has established bidirectional communication between the gut microbiome and the brain via the vagus nerve, with vagal signalling playing a key role in mood and emotional regulation.
Studies demonstrate that disruption of gut-brain vagal signalling is associated with increased anxious thought symptoms, while interventions that improve vagal tone produce corresponding improvements in both gastrointestinal symptoms and anxious thoughts.
This research validates the common scientific observation that gastrointestinal symptoms and anxious thoughts co-occur and respond to the same autonomic interventions.
- Inflammatory markers and anxious thoughts:
Studies in individuals with persistent anxious thoughts document elevated levels of pro-inflammatory cytokines, including IL-6, TNF-alpha, and C-reactive protein, that are inversely correlated with vagal tone.
Interventions that increase vagal tone, including VNS, produce measurable reductions in these inflammatory markers alongside symptomatic improvement, establishing a neuroinflammatory mechanism for anxious thoughts that responds to autonomic rehabilitation.
- Complementary use alongside breathwork and mindfulness:
Research supports that VNS functions synergistically with breathwork and mindfulness practices, both of which also operate through vagal activation pathways.
Users who combine VNS with these practices show greater improvements in HRV and anxious thought scores than either approach alone, reflecting that Nurosym complements rather than replaces existing wellness practices.

The mechanistic conclusion:
Restoring vagus nerve function through targeted stimulation addresses the physiological foundation of persistent anxious thoughts, including sympathetic overdrive, impaired threat-response regulation, neuroinflammation, gut-brain axis disruption, and impaired sleep architecture, rather than managing anxious thoughts as a purely psychological phenomenon without addressing their biological substrate.
VNS Devices as a Solution: How They Work
The Technology Revolution
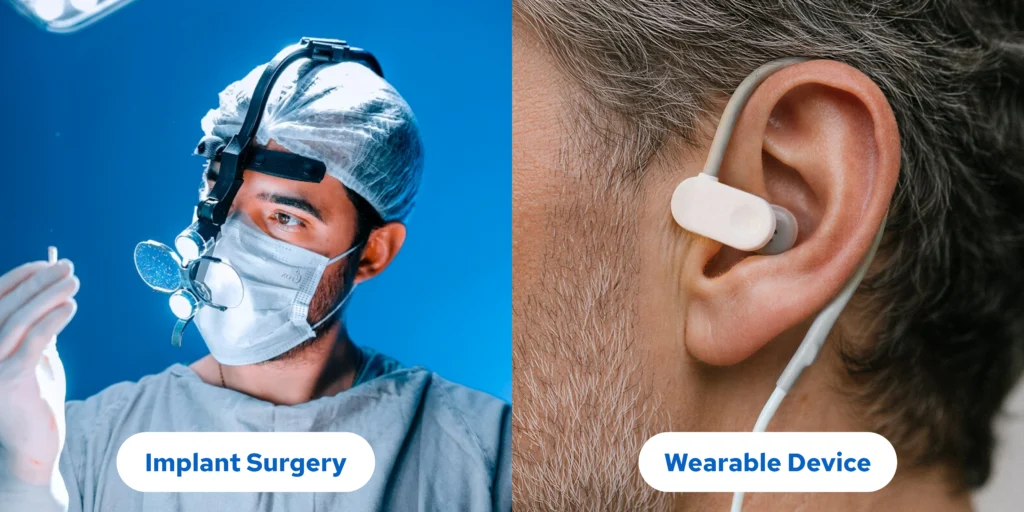
Until recently, vagus nerve stimulation required invasive surgical procedures, implanting electrodes directly on the nerve through operations that carried significant risks, extended recovery periods, and permanent device placement. This confined VNS therapy primarily to therapy-resistant depressive states where the severity of the symptom justified a surgical approach.
Today’s breakthrough changes everything.
Modern transcutaneous vagus nerve stimulation (tVNS) delivers the same therapeutic electrical impulses to the vagus nerve, facilitating neuroplastic adaptation and genuine restoration of autonomic tone, completely non-invasively through the skin:
– No surgery.
– No implantation.
– No recovery period.
– No effort required.
These advanced wearable devices achieve scientifically meaningful effectiveness with an exceptional safety profile, operating through precisely positioned electrodes at two accessible locations:
- Cervically (neck): Targeting the cervical branch of the vagus nerve near the carotid artery, where the nerve runs close to the skin surface.
- Auricular (ear): Targeting the auricular branch of the vagus nerve at the tragus, the only location where cranial nerves reach the body surface, offering direct and precise access without surgical intervention.
This represents a fundamental shift: vagus nerve stimulation therapy that was once confined to operating rooms is now available for daily home use, with scientific-grade precision and zero surgical risk.
Mechanism of Action
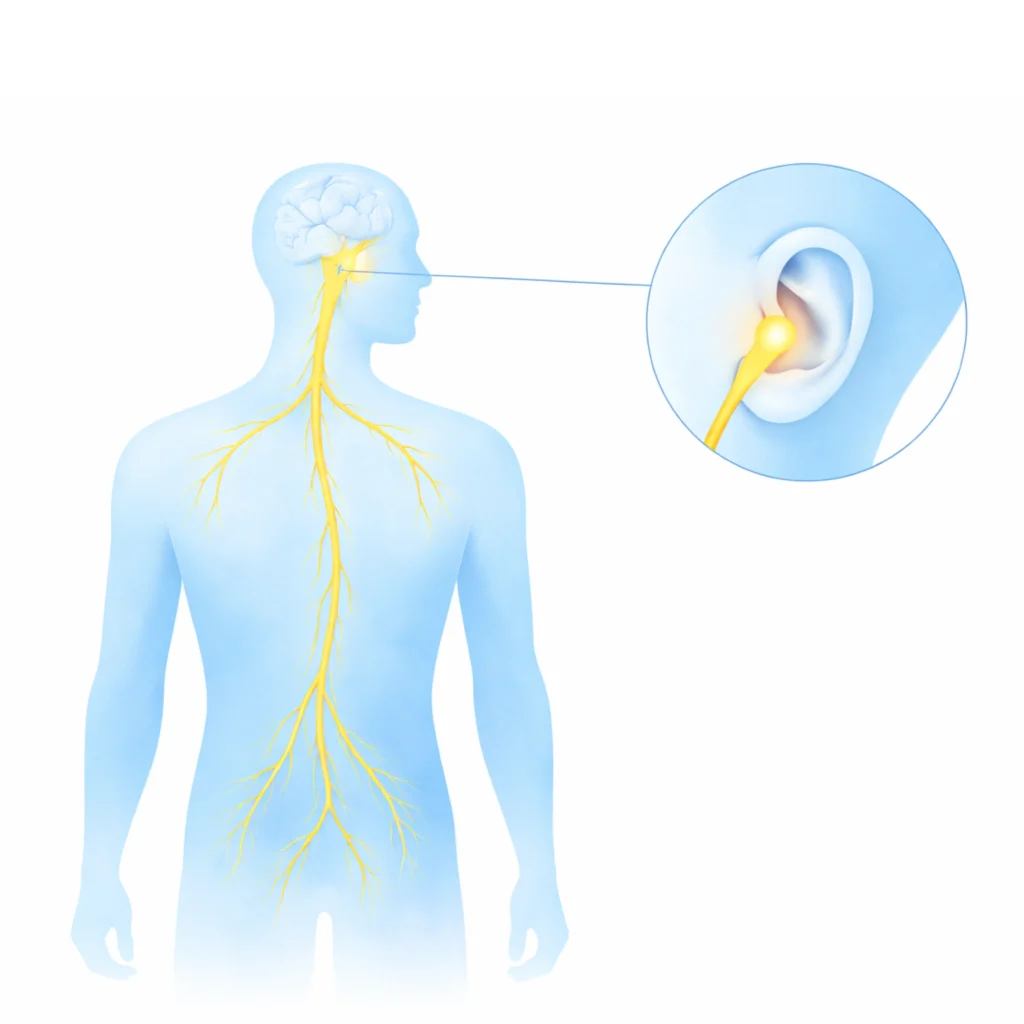
When precisely calibrated electrical impulses reach the vagus nerve, they initiate a cascade of neurophysiological responses directly relevant to anxious thoughts:
- Amygdala modulation: Afferent vagal signals project to the nucleus tractus solitarius in the brainstem, which communicates directly with the amygdala, the brain’s threat-detection centre. Vagal stimulation reduces amygdala hyperactivity, lowering the baseline of perceived threat and reducing the frequency and intensity of anxious thought generation.
- Neurotransmitter modulation: Stimulation triggers the release of acetylcholine at parasympathetic terminals, directly counteracting sympathetic dominance. It also promotes the release of GABA, the primary inhibitory neurotransmitter, and noradrenaline via the locus coeruleus, improving the brain’s capacity to regulate its own arousal level.
- Autonomic rebalancing: Consistent stimulation protocols facilitate a measurable shift from sympathetic dominance towards parasympathetic restoration, improving HRV, lowering resting heart rate, relaxing muscle tone, and creating the physiological symptoms that the brain reads as safety.
- Anti-inflammatory pathway activation: Vagal stimulation activates the cholinergic anti-inflammatory pathway, reducing pro-inflammatory cytokine production, including TNF-alpha, IL-1beta, and IL-6, that contributes to the neuroinflammatory substrate of persistent anxious thoughts.
- Sleep architecture improvement: VNS suppresses sympathetic arousal during sleep, increases slow-wave sleep proportion, and reduces the nocturnal physiological activation that produces racing thoughts at bedtime and early morning waking.
Scientific Parameters
Research-validated VNS protocols for anxious thoughts typically employ:
- Session duration: 30 to 60 minutes daily, allowing for sustained neurophysiological effects and cumulative autonomic adaptation.
- Intensidad: Individualised to sensory threshold, perceptible but comfortable stimulation. Strong enough to activate vagal afferents, gentle enough to avoid triggering a stress response in a nervous system that is already sensitised.
- Consistency: Daily application for a minimum of 8 to 12 weeks. Neuroplastic change and genuine autonomic recalibration require sustained intervention. The nervous system learns safety through repeated experience, not single exposures.
- Complementary use: VNS works synergistically with breathwork and mindfulness. Using Nurosym during or immediately before these practices amplifies their effect by priming the parasympathetic nervous system for activation.
Expected Timeline
VNS promotes gradual nervous system adaptation rather than immediate symptom suppression. For individuals with persistent anxious thoughts, this distinction is important: the goal is not to numb the nervous system but to recalibrate it towards a genuinely lower baseline of physiological arousal.
- Week 1 to 2:
Enhanced sense of calm during and after stimulation sessions. Mild reduction in resting muscle tension. Slight improvement in the ease of falling asleep. Early improvements in HRV detectable on wearable trackers.
- Week 3 to 4:
Noticeable reduction in the physical baseline of anxious thoughts: lower resting heart rate, reduced gastrointestinal symptoms, improved sleep onset. Thoughts remain present but the physical urgency behind them begins to soften.
- Month 2 to 3:
Sustained reductions in anxious thought frequency and intensity. Improved emotional regulation and resilience to stress. Better sleep quality with measurably longer restorative stages.
Reduced physical symptoms of sustained arousal including tension, headaches, and gastrointestinal complaints.
- Month 3 and beyond:
Restored autonomic baseline supporting genuine felt safety. Measurable HRV gains reflecting nervous system recalibration. Improved capacity for social engagement, focused work, and restful sleep.
Reduced reliance on avoidance behaviours and reassurance-seeking strategies. The anxious thoughts that were previously constant become less frequent, less intense, and easier to release.
Safety Considerations
VNS using transcutaneous approaches is generally well-tolerated in scientific research. Potential transient responses may include:
- Mild tingling sensation at the stimulation site during use
- Temporary muscle tension in the neck region with cervical devices
- Brief lightheadedness in initial sessions, typically resolving with protocol adjustment
Note for individuals with anxious thoughts: the novel physical sensation of stimulation may initially heighten physical awareness, which some users find activating.
Beginning at lower intensity settings and building gradually over the first week reduces this likelihood significantly. The sensation normalises quickly with repeated use.
Important limitations: Not appropriate for individuals with cardiac pacemakers, recent acute cardiac events, pregnancy, or a history of vagotomy. Health professional consultation is essential prior to initiating any VNS protocol.
Top 4 VNS Devices for Anxious Thoughts
#1: Nurosym

Price: 700 EUR (Varies by region, with a 40 EUR research subsidy available)
Type: Auricular (ear-worn)
Technology: AVNT by Parasym
Why #1:
- Most extensively validated: Supported by 50 or more peer-reviewed publications from Harvard Medical School, UCLA, and leading research institutions worldwide. No other wearable VNS device approaches this evidence base for any symptom category, including anxious thoughts.
- Directly documented efficacy for anxious thoughts: Scientific studies using AVNT technology document significant reductions in anxious thought severity alongside an 18% improvement in HRV, providing directly relevant evidence for this symptom rather than generalised autonomic improvement.
- 0 serious adverse events in studies to date: For individuals with anxious thoughts, who are typically sensitive to physical interventions and prone to monitoring bodily sensations, this safety record is particularly meaningful.
- Independent certification: CE-marked as a wearable device meeting rigorous safety and performance standards, verified by independent third-party assessment.
- Scientific adoption at scale: Used by 1,000 or more health professionals and researchers. Integrated into institutional protocols. More than 4,000,000 supervised stimulation user sessions completed.
- Complementary by design: Nurosym is documented to work synergistically with breathwork and mindfulness practices, the two most evidence-supported behavioural approaches to managing anxious thoughts. Rather than replacing existing strategies, it amplifies their effectiveness.
- Comprehensive user support: 30-day evaluation period, science-based guidance resources, and responsive technical support from a team grounded in scientific research.
Ideal para: Individuals with persistent anxious thoughts who want the most scientifically validated wearable device available, particularly those whose anxious thoughts have a strong physical component, those who have found cognitive approaches alone insufficient, and those looking to address the autonomic root of their symptoms rather than manage the thoughts themselves.
#2: Truvaga Plus

Price: $544 or more (Device $499, plus conductive spray $45 per year, plus potential subscription costs)
Type: Cervical, neck-held, handheld
Shares core technology with gammaCore, an FDA-cleared device for headache and cluster headache. Delivers rapid parasympathetic effects through the cervical vagal branch and follows a straightforward protocol.
Considerations:
- Ongoing costs for conductive spray and potential app subscription add up considerably over time.
- Known adverse effects include muscle spasms, facial droop, lip pull, and localised headache in a subset of users.
- Not suitable for individuals with cardiac symptoms, pacemakers, or recent cardiovascular events.
- Mobile app connectivity issues have been reported. FDA clearance is for headache, not for anxious thoughts or autonomic dysregulation.
- For individuals with anxious thoughts who are sensitive to unexpected physical sensations, the facial muscle effects reported by some users may be activating rather than calming.
Ideal para: Those who prefer cervical stimulation with an FDA-cleared technology lineage and can tolerate the potential for facial muscle adverse effects.
#3: Pulsetto

Price: $350 to $371 (Device $269, plus conductive gel $81 to $102 per year)
Type: Cervical, hands-free collar
Offers a hands-free wearable design, HSA and FSA eligibility, and a 2-year warranty.
Critical limitations:
No scientific studies demonstrating efficacy for anxious thoughts, autonomic dysregulation, or any chronic symptom, only company press releases and retail testimonials.
Frequent fit problems create inadequate nerve contact, particularly for individuals with smaller necks. For individuals with anxious thoughts who have already tried multiple approaches without adequate results, the absence of scientific validation is not a minor consideration.
Users managing anxious thoughts consistently report minimal to no measurable improvement compared to research-validated devices.
Not recommended for persistent anxious thoughts:
The price difference appears attractive until you factor in the cost of continued symptoms without measurable improvement. When anxious thoughts are already affecting work, relationships, and quality of life, the absence of an evidence base matters.
#4: Sensate

Price: $299 to $349
Type: Chest-worn vibrotactile device, not true VNS
A comfortable pebble-shaped device worn on the chest. Simple app interface with accompanying soundscapes. Lower price point. Designed for use whilst lying down or resting.
Critical distinction: Sensate does not stimulate the vagus nerve through electrical impulses. It uses infrasonic vibrations and bone conduction at the sternum, an indirect approach targeting general relaxation rather than specific vagal nerve activation.
For general stress reduction in otherwise healthy individuals, this may provide some benefit. For individuals with persistent anxious thoughts driven by genuine autonomic dysregulation, it does not address the underlying mechanism.
The distinction matters because anxious thoughts are not simply a relaxation deficit.
They reflect a nervous system with structurally impaired self-regulation capacity.
Genuine vagal rehabilitation, of the kind documented in the scientific literature, requires targeted electrical stimulation of the vagal nerve pathway, not vibrotactile stimulation of the sternum.
No scientific studies demonstrate Sensate’s efficacy for anxious thoughts or autonomic symptoms, only company-funded studies showing mild stress reduction in healthy volunteers.
Ideal para: Those seeking a gentle relaxation and wind-down tool as one component of broader symptom management. Not recommended for individuals prioritising evidence-based therapy for persistent anxious thoughts.
Conclusion:
Nurosym offers the most comprehensive scientific validation, directly documented efficacy for anxious thoughts, a safety record of 0 serious adverse events in studies to date, synergistic compatibility with existing wellness practices, and the strongest evidence base for individuals who are ready to address the autonomic root of their anxious thoughts rather than manage the thoughts themselves.
Anxious Thoughts and Sleep Problems

For the majority of individuals with persistent anxious thoughts, the bedroom is the most difficult room in the house.
The reduction of external demands and distractions that sleep requires does not quiet the nervous system…
It amplifies it:
– Racing thoughts
– A heightened awareness of physical sensations
– An inability to shift out of physiological arousal combine to make sleep onset effortful, sleep maintenance unreliable, and waking unrefreshing.
The vagal connection is direct and well documented.
Vagal tone is the primary physiological driver of the transition from wakefulness to restorative sleep. When it is impaired, the nervous system lacks the mechanism to down-regulate sympathetic activation sufficiently for sleep to begin and for its restorative stages to be sustained.
Research shows that individuals with persistent anxious thoughts have measurably reduced slow-wave sleep and REM sleep, the stages in which emotional processing, memory consolidation, and physical repair occur.
This is why standard sleep hygiene advice provides incomplete relief for individuals with anxious thoughts. The advice addresses the context of sleep without addressing the neurological reason it fails.
Telling a person with low vagal tone to avoid screens before bed and keep a consistent sleep schedule is not wrong. It is simply insufficient to override the physiological state that is preventing them from sleeping.
And here’s what is surprising:
Studies using Nurosym’s AVNT technology have documented improvements in sleep architecture alongside reductions in anxious thought severity, including increased slow-wave sleep proportion and reduced nocturnal sympathetic activation.
For individuals whose sleep problems and anxious thoughts are part of the same autonomic pattern, addressing vagal tone addresses both simultaneously through a shared mechanism.
Anxious Thoughts and Heart Palpitations

One of the most distressing physical features of persistent anxious thoughts is heart palpitations: the sudden, intrusive awareness of a rapid, irregular, or forceful heartbeat that occurs at rest, without exertion, and without apparent cause.
For many individuals with anxious thoughts, palpitations trigger a secondary wave of fear that the heart is in danger, escalating physiological arousal and deepening the anxious episode.
The mechanism is autonomic.
The vagus nerve is the primary parasympathetic regulator of heart rate.
When vagal tone is low, the heart rate becomes difficult to regulate, rising more easily in response to minor triggers and returning to baseline more slowly afterwards.
Heart rate variability decreases. The cardiac rhythm becomes less flexible, more reactive, and more prone to the palpitation episodes that many individuals with anxious thoughts find among their most frightening symptoms.
But here is what is interesting:
Research consistently documents that individuals with persistent anxious thoughts exhibit significantly reduced HRV, reflecting exactly this pattern of reduced parasympathetic cardiac control.
Studies using transcutaneous auricular VNS have documented measurable improvements in HRV and reductions in resting heart rate alongside symptomatic improvements in anxious thoughts, confirming that cardiovascular regulation and the subjective experience of anxious thoughts respond to the same vagal intervention through the same mechanism.
For individuals whose anxious thoughts are significantly driven by awareness of their own heart rate and palpitation episodes, restoring vagal tone through VNS addresses the physical trigger of these episodes directly, rather than simply encouraging the individual to reinterpret their heart rate as non-threatening.
Take Action
Persistent anxious thoughts are not a personal failing, a sign of weakness, or evidence that you are unable to manage ordinary life.
For a growing number of researchers and health professionals, they are increasingly understood as a measurable consequence of vagal impairment and autonomic dysregulation, symptoms with an evidence-based approach to rehabilitation that goes beyond managing thoughts and directly addresses the physiological state generating them.
Your autonomic nervous system possesses the capacity for neuroplastic adaptation.
The nervous system that learned to stay alert can be supported, through consistent and targeted stimulation, to learn what safety feels like again.
With backing from 50+ scientific studies, independent CE-marking certification, a safety record of 0 serious adverse events in studies to date, and more than 4,000,000 documented stimulation user sessions worldwide, Nurosym provides the most scientifically validated approach available for individuals with persistent anxious thoughts who are ready to address the root cause.
Disclaimer: This article has been written by a licensed medical professional and is intended for general informational purposes only. It does not substitute for personalised medical advice, diagnosis, or therapy. Readers should always seek the guidance of a qualified health professional with any questions regarding a medical symptom or health objectives. Never ignore or delay seeking medical advice based on information presented here.
Fuentes
- Thayer JF, Ahs F, Fredrikson M, Sollers JJ, Wager TD. A meta-analysis of heart rate variability and neuroimaging studies: implications for heart rate variability as a marker of stress and health. Neuroscience and Biobehavioural Reviews. 2012;36(2):747 to 756. https://doi.org/10.1016/j.neubiorev.2011.11.009
- Breit S, Kupferberg A, Rogler G, Hasler G. Vagus Nerve as Modulator of the Brain-Gut Axis in Psychiatric and Inflammatory Disorders. Frontiers in Psychiatry. 2018;9:44. https://doi.org/10.3389/fpsyt.2018.00044
- Roque Bravo R, Faria AC, Brissos S, Baptista Luiz J, Trigo Pereira C, Matias Dias C, Figueira ML. Transcutaneous vagus nerve stimulation in the management of therapy -resistant anxious thoughts: a systematic review. Frontiers in Neuroscience. 2022;16:968590.
- Porges SW. The polyvagal theory: neurophysiological foundations of emotions, attachment, communication, and self-regulation. New York: Norton; 2011. https://psycnet.apa.org/record/2011-04659-000
- Kaniusas E, Kampusch S, Tittgemeyer M, et al. Current Directions in the Auricular Vagus Nerve Stimulation I: A Physiological Perspective. Frontiers in Neuroscience. 2019;13:854. https://doi.org/10.3389/fnins.2019.00854
- Tracey KJ. The inflammatory reflex. Nature. 2002;420(6917):853 to 859. https://doi.org/10.1038/nature01321
- Dinan TG, Cryan JF. The microbiome-gut-brain axis in health and disease. Gastroenterology Clinics of North America. 2017;46(1):77 to 89. https://doi.org/10.1016/j.gtc.2016.09.007
- Bonaz B, Bazin T, Pellissier S. The Vagus Nerve at the Interface of the Microbiota-Gut-Brain Axis. Frontiers in Neuroscience. 2018;12:49. https://doi.org/10.3389/fnins.2018.00049
Compartir a través de:


